
Insights into the Treatment of Children with Down Syndrome
. . . and other Children with Muscular Hypotonia
In his capacity as a physician, therapist and fellow human being, Dr. Rodolfo Castillo Morales spent more than 40 years of his life accompanying people with down syndrome. This gave him a wealth of experience that only few physicians had. The oldest of his more than 4,000 patients with down syndrome were over 40-years-old. As a physician who mastered Bobath and Vojta therapy, he found something lacking in the treatment of children with muscular hypotonia. The lack of a more effective means of helping these children inspired him to develop his own treatment concept. During our many years of working intensively together with Dr. Castillo Morales, we educational therapists had an opportunity to acquire a deep understanding of his concept. Our aim now is to transfer this knowledge to other therapists and to share it with parents and children.
The Castillo Morales® concept begins with a holistic examination of children with down syndrome in their family settings and in their broader environments, including kindergartens and schools, and also seeks to counteract secondary pathologies. The joint and continuous identification and expansion of channels of communication is regarded as a prerequisite for meaningful dialogue and smooth interaction. Numerous verbal and non-verbal approaches to deepening the understanding of the parties involved are used at all levels and in accordance with the individual needs and abilities of the developing children.

The affected children often exhibit numerous distinctive bodily characteristics(e.g. short arms, open mouth and protruding tongue) and functional limitations (e.g. lack of activity control owing to a genetically determined maturation disorder; see The Castillo Morales Concept, 2012, Chapter 3.2). The provision of comprehensive accompaniment and assistance therefore makes sense for a number of these children and their parents, for instance, shortly after birth in case of sucking difficulties. A trained Castillo Morales® therapist is able to competently intervene at this early juncture to ensure that feeding is as sufficient, pleasurable and effortless as possible.
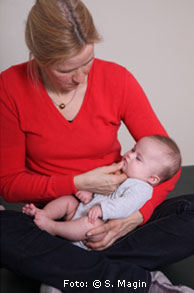
Therapists are able to both advise and support the parents and to undertake therapeutic measures in dialogue with the child to enable and facilitate appropriate sucking in light of the circumstances, abilities and needs of the child and the child’s family. In the image we see Lisa who, held cozily and securely down to her feet, is able to optimally deploy her muscles to efficiently and pleasurably suck at her mother’s breast.
Another approach might involve drinking from a training cup in children who cannot be motivated to suck after negative neonatal and early-childhood experiences. If this vital need goes unmet, the focus of therapy can be shifted towards communication (verbal and nonverbal), sensorimotor development and the additional acquisition of the skills necessary for eating and drinking so that the children learn to participate as well and as independently as possible in everyday activities. Paying attention to and promoting visual perception plays a significant role in this connection.
The scope of the therapy is limited to the phased provision of specific forms of support that correspond to the particular needs and circumstances of the child and the child’s family. The therapeutic intervention is not conceived as a permanent arrangement. Dr. Castillo Morales regarded his concept as a reflection of life itself. This is why we work in the presence of and in cooperation with the parents on the development of the children’s capacity to participate in everyday activities. Careful observation and open dialogue with the parents enables us to gain a better understanding of the children’s abilities. Working from a basis of trust and respect, we develop necessary and optional forms of support for daily activities. In individual cases, it may be beneficial to have a specialist fit the child with a palatal plate.
The therapeutic measures vary considerably and always provide an opportunity for verbal and non-verbal (physical) communication between the therapist or other caregivers and the child. Among the many techniques in the therapist’s repertoire, manual vibration in various individually adapted intensities and frequencies together with the application of traction and pressure to certain sensorimotor zones of the body has emerged as especially effective. The technique enables an intensification of the children’s muscle activity, ranging as far as the orofacial complex, and also directs their attention to important sensory zones. Close body contact belongs to the therapists’ work, as it allows them to immediately detect every change in muscle tone, every motor impulse, every action and reaction, and to respond accordingly in a continuous process of adapting to the needs of the children and encouraging development. The children remain securely ensconced in a holistic form of dialogue. This is because “communication is the key to the child’s soul” (RCM),and therefore the basis of our actions.
On the following pages, we see pictures of children in reference positions that can be used and expanded upon to optimize the efficiency of the muscular activation, function and coordination. The names of the children have been changed to protect their identity.


In this position, L. experiences borders through her contact with the body of the therapist. This introduces the possibility of lifting her arms and legs against the force of gravity. L.’s sitting bones are placed against the therapist’s stomach and her feet against the therapist’s ribcage. The individualized stimulation of a sensorimotor zone on the sternum via the application of vibration and traction and the tractive force applied to the back of her head enable L. to control her hands and operate on the therapist’s hand, lift her arms and play with her fingers. L.’s overall muscle activity is so elevated in this situation that she also exhibits a clear increase in muscle tone in the orofacial region.
The bracing activity of the feet seen here is therapeutically supported via vibration, traction and pressure applied to sensorimotor zones. Children with hypotonia tend to use their feet to touch things as opposed to using them to brace themselves. This is why it is important to work on symmetric and asymmetric (always involving rotation) foot bracing activities.

This leads to initial attempts on the part of the children to shift their weight laterally. These movements play a special role. Although they are more difficult for these children to execute, they are a basis for movements that will lead to an improved and variable control over posture and locomotion. Moreover, they will also permit a gradual exercising of lateral and rotational lower jaw movement that is so important for the development of chewing.
In the image we see L. engaged in a calm sensorimotor dialogue on my lap as I provide gentle jaw support. It is important here to avoid provoking lower jaw protrusion. This position again creates an opportunity for L. to generate tension with her feet. Her sitting bones find support on my thigh. Using my elbow I’m able to secure a straightening of the cervical spine. This also has a positive effect on the active backwards placement of the tongue and the active closure of the jaw and mouth.
Image 4: H. in assisted upright sitting position
Remaining in reclining positions over extended periods of time can lead to lower cognitive performance (Dr. R. Castillo Morales, 1997). We verticalize children as early as possible and offer them weight-bearing opportunities for the feet so that they can discover the world from a higher vantage point. Doing so has the effect of increasing the children’s contact with their environment and promoting a greater degree of alertness and willingness to try out more things.

In this case, H. is actually conversing with her mother (not shown in the picture). The horseshoe cushion enables her to send herself impulses that encourage proper posture and alignment via the supporting activity of her hands. Her sitting bones find pivotal support on my thigh and her feet brace against the floor to secure more support. This allows H. to increase the long-chain muscle activity that supports an upright position. This posture and alignment control (capacity of the body to establish a proper physiological arrangement of the individual body segments) is also an important prerequisite for deeper breathing, straightening of the cervical spine, enhanced jaw and mouth closure, and an unburdened capacity to drink, swallow and eat. During the session, I use my hands to apply pressure and individually adapted vibratory and tractive forces to sensorimotor zones of the back and shoulders.

Image 5: H. in horseshoe seat
In the picture we see H. in a functionally asymmetric position: the horseshoe cushion compensates for her short arms, enabling her to support herself in an asymmetric position. I work on H.’s viewing height so that we can encounter one another at the same level and communicate. This also helps her to avoid overextending her cervical spine and to remain in a position of proper physiological alignment. The exercise facilitates mouth closure and also encourages a backwards displacement of the tongue.
The asymmetric sitting positions create an important basis for increased muscle activity. As already mentioned, they permit the children to execute rotational movements with the lower jaw, thereby helping them to acquire better chewing skills. During the session, I use my hands to apply pressure and individually adapted vibratory and tractive forces to key sensorimotor zones.
Image 6: H. in horseshoe seat with gentle jaw support
Here, I use a gentle jaw-control maneuver to allow Hanna to practice closing her mouth. With my other hand, I apply pressure and vibratory and tractive forces to a key sensorimotor zone while at the same time helping H. to support herself and maintain a proper upright position.


Image 7: L.
My sitting position is elevated so that L. can sit on me and maintain a proper upright position, i.e. actively using his feet for support and his right hand to brace himself. I stimulate sensorimotor zones by applying pressure and vibratory and tractive forces to activate diagonal muscle chains and help L. to improve his ability to shift his weight laterally and gain greater control over his posture.
The elevated muscle tension that arises enables L. to more effectively close his mouth and execute lateral and rotational movements with his lower jaw. This optimally supports activities such as eating (chewing), drinking, and swallowing.
The immediate environment in which the children find themselves plays an important role in permitting the kind of muscle activation that is necessary for vital activities such as talking, moving, assuming an upright posture, playing, eating and drinking. Sitting on a chair with a wedge-shaped cushion enables the children to execute efficient support and bracing movements with their feet and right elbows. The chair is turned slightly toward the table so that L. can orient himself toward the table from his center (asymmetric weight shifting with spinal rotation). The impact of this more active approach to positional control can be seen ina full range of muscle groups, including the orofacial complex.

… More active and alert position

“We join the children in their daily lives, we let them move their hands freely when they are ready to be autonomous and to decide on their own that it is time to say goodbye.”
Dr. Rodolfo Castillo Morales
Author: Susanne Magin, Physiotherapist, Educational Therapist for the Castillo Morales® Concept